
A Third of Eligible Migraine Patients Were Not Offered preventive therapy
Find out why a third of eligible migraine patients were not offered preventive therapy and
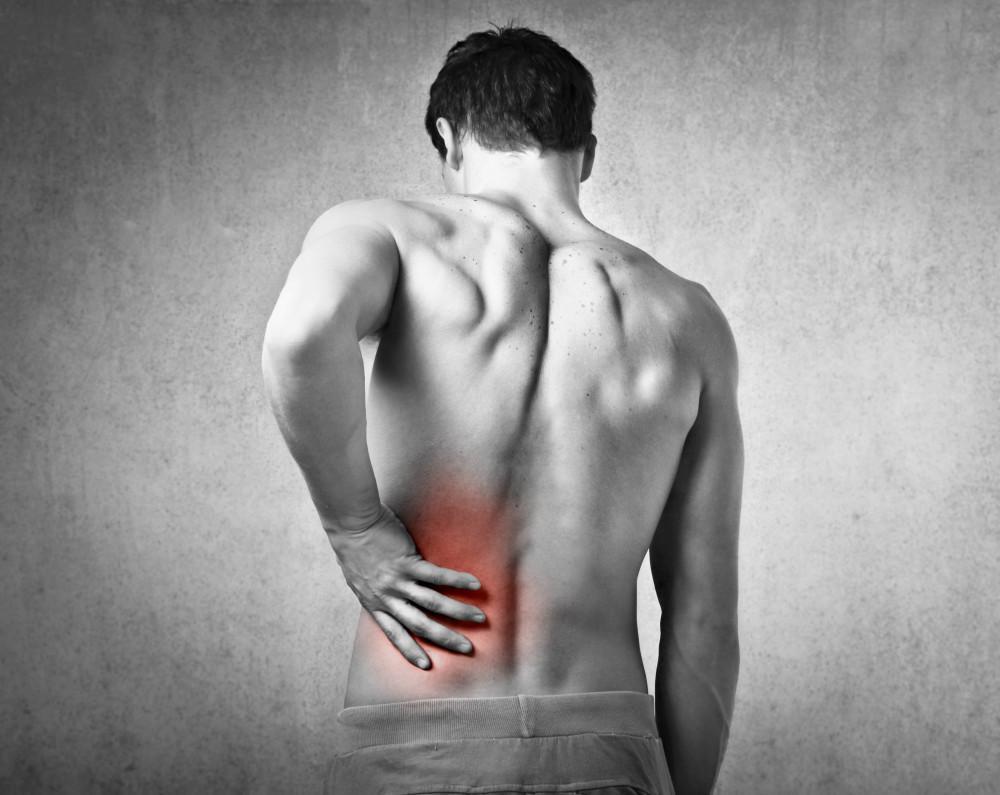
Back pain commonly results from injury, compression, or misalignment of joints in the back. Facet joints connect the back’s vertebrae, guiding their range of motion and allowing movement such as bending over and extending the back. The sacroiliac joint connects the sacrum bone of the lower back with the pelvis. When either facet joints or the sacroiliac joint are damaged, compressed, or misaligned, an individual may experience pain and inflammation in the surrounding area that limits mobility and quality of life. This condition can be acute, occurring intermittently for a short period of time, such as when a person exerts themselves, or chronic, with pain and limited mobility occurring for an extended period of time or even continuously. The pain may be mild or severe, and this influences decisions regarding the optimal treatment path.

A number of treatment options exist for back pain resulting from issues affecting the back’s joints. These span the gambit from oral medications to minimally invasive injections to surgical procedures. The optimal treatment will depend on the nature and severity of the problem along with an analysis of the risks and benefits the treatment may provide to an individual considering their personal medical history and profile. Medications may include analgesics such as ibuprofen and muscle relaxants. A number of injections are available as well, including injections of local anesthetics, anti-inflammatory medications, joint blocks, and Botox. When these options fail to control the condition, many patients consider a more invasive surgical approach. However, it is important for sufferers of back pain to be aware of another minimally-invasive option: radiofrequency joint ablation.

When back joints are damaged or compressed, pain signals from the area travel to the brain via the nervous system informing the body and mind that something has gone wrong. Pain signals from the facet (back vertebrae) joints are carried by medial branch nerves and from the sacroiliac (hip-lower back) joint by lateral branch nerves. Radiofrequency ablation is a technique that inhibits pain signals by disrupting the ability of these nerves to conduct them, thus reducing the pain experienced by the patient. Medial and lateral branch nerves are not responsible for sensation or muscle control in the arms and legs, limiting negative side effects from this disruption. Radiofrequency ablation of the lateral and medial branch nerves is minimally invasive and can be highly effective in a large proportion of patients.
Before a patient undergoes radiofrequency ablation, they will first receive a joint block injection in the facet or sacroiliac joints to determine whether the pain is indeed being communicated by the medial or lateral branch nerves. This procedure itself may be effective in reducing or eliminating the pain being experienced. The radiofrequency ablation process begins with the injection of a local anesthetic in order to limit potential discomfort from the procedure. The nerves affected are numbed. Using the x-ray guidance of a fluoroscopy machine, the physician will insert a special radiofrequency needle into the targeted areas. A radiofrequency current runs through the needle, disrupting the ability of the targeted nerves to transmit pain signals. Following the procedure, there is a 1-2 hour recovery period after which the patient will be able to resume daily activities. Pain relief from this procedure is commonly substantial and can last between 6 months and a year.
If you suffer from back pain and want to know if radiofrequency ablation is right for you, contact New York Neurology today.
NY Neurologists

A Third of Eligible Migraine Patients Were Not Offered preventive therapy
Find out why a third of eligible migraine patients were not offered preventive therapy and

New NYNA Tourette Syndrome Study
Learn how NY Neurology Associates is advancing Tourette syndrome care with innovative treatments and a

Seizures: Understanding and Overview
Discover what causes seizures, how to recognize key symptoms, and the steps that help keep
